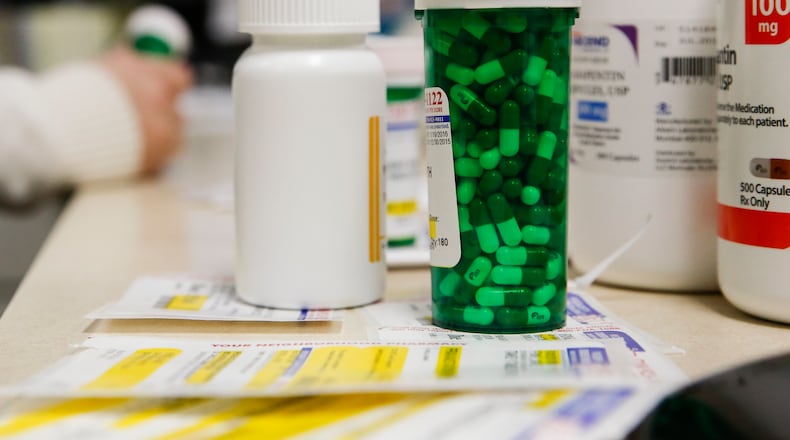
When Ohio Medicaid pays for prescription drugs, the money flows through the middlemen, who process claims and negotiate prices on prescriptions.
Catching up? Read our latest pharmacy reporting here:
• Pharmacy middlemen made $223.7M from Ohio Medicaid
• With small pharmacies disappearing, Medicaid cuts seen as culprit
• DeWine anticipates ‘major litigation’ against pharmacy middlemen
The privatized system kept the state’s Medicaid spending contained and predictable. CVS Caremark, one of the pharmacy benefit managers, highlighted that Ohios Medicaid spends per prescription 13 percent less than the collective average costs of states that manage their own program instead of having a privately managed system.
“We remain committed to continuing to work together with the state and the managed-care plans to improve the system, lower drug costs and serve the health care needs of Ohioans,” stated CVS.
Medicaid doesn’t directly pay pharmacists. Ohio Medicaid pays five private insurance companies to manage Medicaid plans for the state. The insurance companies contract out pharmacy benefits to middlemen, which pay pharmacists to fill prescriptions.
However, the middlemen have not previously disclosed how much money they are making off of the privatized system, and pharmacists have said the companies’ profits have come from keeping too much taxpayer money that should go to pharmacies.
The Dayton Daily News reported last year pharmacists were operating on losses on prescriptions filled for Medicaid to the point that some pharmacies with high volumes of Medicaid patients were closing their doors.
Several pharmacists described “take it or leave it” contracts where the pharmacy benefit managers offered pharmacists low rates and no room for negotiation.
Independent pharmacists have also said CVS Caremark has a conflict of interest, because it owns a pharmacy benefit manager and also a chain of retail pharmacies, which compete with independent pharmacies.
MORE: Miami Valley Hospital ranked 4th in Ohio
The auditor report showed 132 independent community pharmacies, 78 small chain pharmacies and 161 large chain pharmacies have closed in Ohio since 2013. However, about 55 of the large chain pharmacies that closed were CVS buying Target pharmacy locations, which are technically recorded as closures but did not mean a reduction in the number of large pharmacies open.
The closure data shows that 48 percent of independent pharmacies that closed since 2013 were in either northwest or northwest Ohio, which is also where pharmacies were paid the lowest reimbursements per drug.
The report said the data “coincides with concerns expressed by pharmacists regarding reductions in reimbursements. However this data does not show causality and further research is needed to determine the factors that led to these closures.”
CVS said the auditor’s report doesn’t paint the full picture. It stated independent pharmacies make up about 40 percent of all of the pharmacies in its national network and the company has added 63 independent pharmacies in Ohio to its network in the last three years.
This is the first time state agencies are collecting data on how the pharmacy benefit managers do business. It is hard to benchmark the data against other states since other states that use pharmacy benefit managers have not made public similar information.
Ohio Medicaid in June published a report by a consultant that for the first time showed how much the companies are spending on prescriptions and how much of the money they are keeping.
The Ohio Auditor’s report broke down how much the companies are charging for generics verses name-brand drugs and how the amount of money they keep varies by county.
The report shows that the average amount that the pharmacy benefit managers kept was $5.71. That breaks down to $1.85 kept on average for brand-name prescriptions, $6.14 for generics and $33.49 for specialty drugs.
The consultant hired by Ohio Medicaid said based on its information about the market, that out of the money the pharmacy benefit managers kept per prescription, the cost for covering their administrative fees would be $0.95 to $1.90 per prescription.
“Although this figure may not include all of services performed by a (pharmacy benefit manager), it suggests Ohio’s current spread may be excessive and warrants the State taking further action to mitigate the impact on the Medicaid program,” the auditor’s report stated.
The amount of money pharmacy benefit managers retained from Medicaid prescription transactions was highest in the northwest and northeast regions of the state, the report found. The spread on brand drugs in northwest Ohio was 77 percent higher than the statewide average, and northeast Ohio was 69 percent higher.
MORE: Employed but uninsured? In Ohio, you’re not alone
For generic drugs, northwest Ohio was 18 percent higher and northeast Ohio was 19 percent.
The Ohio Auditor stated in its report that “this raises questions as to why pharmacies in these regions are reimbursed at lower amounts for these two drug types.”
When pharmacy benefit managers keep more of the money it invoices the state for generic drugs, it has an outsized impact because generic drugs make up 86.1 percent of Medicaid prescription claims.
“The more we learn, the more troubling this becomes,” Ohio Auditor David Yost said in a statement following the release of the report. “Our review has answered many of the questions presented by state lawmakers, but the lack of information from the (pharmacy benefit managers) limits the depth of our work. Without more information – on what’s happened in the past and what is planned for the future – Ohioans will never know if they’re getting a fair price.”
Yost presented his report to the Joint Medicaid Oversight Committee, which oversees the insurance program for low income Ohioans.
The Dayton Daily News reported earlier this week that Ohio plans to overhaul the way Medicaid pays for prescriptions in the wake of mounting controversy over the pharmacy benefit managers' business practices.
In a letter to the insurance companies, Ohio Medicaid said under the new rules, pharmacy benefit managers will charge the insurance companies exactly what they pay pharmacies for prescription drugs and dispensing fees.
Pharmacy benefit managers would charge an explicit fee for administrative services. The new system will be in place Jan. 1.
CVS stated that under current business model, the money the companies keep is in lieu of a separate administrative fee, and the money funds “vitally important benefit management services” such as clinical and customer support, programs for medication adherence, management of the drug formula, and other services.
THE STORY SO FAR
PREVIOUSLY: Lawmakers have started demanding more transparency on how pharmacy benefit managers do business with Ohio Medicaid. Ohio Medicaid just announced it will overhaul how the the companies get paid, switching to a more transparent system.
WHAT'S NEW: The Ohio Auditor shared a report showing pharmacy benefit managers passed along less Medicaid money to pharmacists for generic drugs than for brand name drugs.
WHAT'S NEXT: Ohio's privately managed Medicaid plans will need to have cancel their current contracts with pharmacy benefit managers and form new contracts using a more transparent business model by Jan. 1.
About the Author