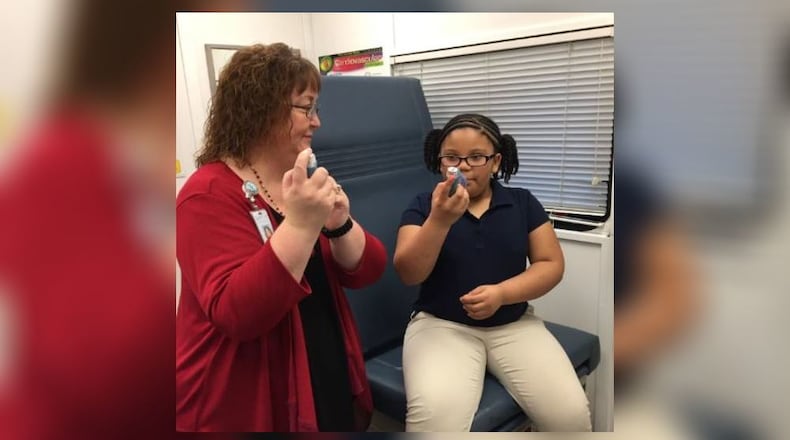
When the program was first started, the No. 1 reason that Dayton schools would call for an ambulance was an asthma or respiratory related problem.
PREVIOUS COVERAGE: New alliance targets major child asthma problems
“Also we knew anecdotally that we had a lot of kids who were in the nurse’s office, out of the classroom. They’re not learning and progressing if they’re in the nurse’s office having severe asthma issues,” said Lisa Montgomery, nurse with Dayton Public Schools.
To address the health issue, Community Health Centers of Greater Dayton and Dayton Public Schools, with the help of a $125,000 grant from CareSource Foundation, brought a sidelined RV back to life as a mobile health unit.
The mobile health unit staff go to the different schools and for children who have signed consent forms they provide asthma well-checks, treatment for attacks, asthma action plans, education, care coordination and referrals for services.
Montgomery said they didn’t want to duplicate work by a child’s primary care provider but found there was a need for children to learn how to use an inhaler and know how to manage asthma flare ups.
“One of the things we honed in on was that there are basic skills students need to have in order to use their medication properly and effectively, and to manage their asthma effectively. So that became our primary goal was to enhance asthma self management skills,” she said.
Asthma triggers at home and at school can range from mold to dust mites to tobacco smoke. In the city of Dayton, there are triggers like air pollutants from the concentration of highways to environmental triggers from older housing.
The program has reduced asthma-related school absences and dramatically reduced asthma-related emergency department visits and inpatient hospitalizations, according to data analyzed by CareSource.
The study selected 183 students as the intervention group and another 574 students with similar demographics as the control group. By comparing records from 12 months before and after the launch, the final numbers showed more than $100,717 in emergency room savings, $126,149 in inpatient savings and $28,878 in other savings between Jan. 1 2017 and Dec. 31 2017, CareSource reported.
MORE: High-fives, busing issues greet students on first day of school
This mobile health unit builds on the work Community Health Centers of Greater Dayton is already doing in Dayton. The health center has a sliding-fee system based on income and helps make health care accessible for low-income or uninsured patients. Five of its six health center locations are also in the Dayton Public Schools district, which is a majority low income student population.
“We’re already seeing them as their primary care provider in some cases, so it really fits what we’re doing,” Gregg Hopkins, executive director of Community Health Centers of Greater Dayton, said.
Besides the mobile health unit, the district is also doing asthma education in their schools with the Open Airways Program, which is a school-based asthma education program, and they are working with teachers and staff so they know how to recognize symptoms.
“Because sometimes young students don’t recognize the early symptoms,” Montgomery said.
Dayton schools and Community Health Centers are also part of the Dayton Asthma Alliance, which is a collaboration of different community groups such as Dayton Children's Hospital that are all working on improving the health of children with asthma.
MORE: Free DPS high school busing plan starts Monday, improves Sept. 30
“The mobile health unit is just one component of a whole asthma approach that’s happening,” Montgomery said.
School-based health approaches are great ways to break down silos and make children’s health care holistic and accessible by bringing services right to the children, said Loren Anthes, public policy fellow at Cleveland-based Center for Community Solutions, who has researched school-based health care initiatives.
While there is a tangible benefit to school-based health care, Anthes said it can also be difficult to get a program started.
“It’s not that people don’t think it’s valuable. The challenge is often that it’s not profitable enough for providers to get involved,” Anthes said.
But when school-based programs are in place, they can help students learn because they help address problems that are beyond a student’s control that could be getting in the way of learning.
“If you can’t control your asthma, and or you can’t see the chalkboard, or you have some other sort of issue going on, that could be easily remedied just by a simple conversation with a doctor. The power of that is immense,” Anthes said. “This sort of investment produces better outcomes for kids.”
Mobile Health Unit results
$100,727: Adjusted total ER savings
$126,149: Adjusted total inpatient savings
$28,878: Other savings
1.96: Return on initial $125,000 investment
Source: CareSource
About the Author