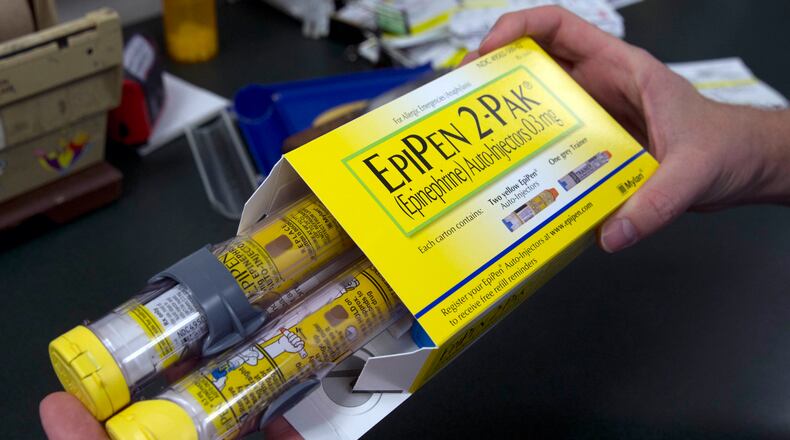
Pharmacy benefit managers (PBMs) serve as middlemen between insurers, pharmacies and manufacturers. They negotiate lower prices for insurers, but have been criticized for keeping secret how much of those negotiated rebates they are keeping.
RELATED: Consumers kept in dark over drug pricing
Drug companies have incentives to raise prices, according to the lawsuit, in order to give larger rebates to the PBMs who then pocket significant revenues and don’t pass the savings along to patients.
PBMs dispute this claim, saying they do pass along the significant savings they negotiate.
“PBMs such as CVS Caremark help to lower drug costs by employing market competitive principles to drug manufacturer pricing that result in real cost savings for clients in the form of rebates,” said CVS Health spokesman Michael DeAngelis. “In fact, CVS Caremark passes along more than 90 percent of the price discounts it receives directly to its clients.”
The PBM’s clients are insurers or employers, and the lawsuit contends that those savings never make their way to individuals who are paying more out-of-pocket for prescriptions at the same time prices are on the rise.
“Rising drug benchmark prices are particularly harmful to those in high-deductible plans, who often have trouble affording prescription drugs, and are even forced to forego purchasing needed prescription drugs, due to high annual out-of-pocket costs,” the lawsuit filed in Minnesota in June says. The three main plaintiffs are EpiPen users from Minnesota, Florida and New Jersey.
RELATED: Dayton man lead plaintiff in drug lawsuit alleging price-gouging
EpiPen manufacturer Mylan and other drug companies have faced numerous lawsuits over price increases with some mentioning the role of PBMs, but few suits have named the middlemen as defendants.
“Historically, when it comes to rising prescription drug costs, both public ire and legal battles have been primarily focused on drug manufacturers,” said Antonio Ciaccia, director of government and public affairs for the Ohio Pharmacists Association. “Now, just as patients and policymakers begin to better understand the big hand that PBMs have in raising prescription drug costs, that same evolution seems to have finally made its way to the courts as well.”
Express Scripts has long defended the rebate system, saying that manufacturers alone set drug prices.
“Rebates don’t raise drug prices, drug makers raise drug prices,” said spokesman Brian Henry. “We will vigorously defend ourselves.”
RELATED: EpiPen maker hit with lawsuit alleging price inflation
Prime Therapeutics also said in a statement it believes the lawsuit is withouth merit and will vigorously defend against it.
“This lawsuit is built on a false premise about the role of PBMs,” said DeAngelis with CVS Health. “Nothing in our agreements prevents a drug manufacturer from lowering the prices of their products and we would welcome such an action.”
The argument over who really controls drug prices has intensified as patients become fed up and demanded answers via Congress.
“Federally, this has become a bit of chicken and egg fight between manufacturers and PBMs,” Ciaccia said. “Manufacturers claim that they have to raise prices in order to pay off the PBM. PBMs claim that the manufacturers have total control, and that rebates are their tool to combat rising drug prices. Regardless of who is more in the right, there is no question that this model is in desperate need of an overhaul.”
MORE PRESCRIPTION DRUG PRICES COVERAGE:
Who’s really controlling your drug prices? 5 things to know
Read fine print: Prescription drug discounts may contain catch
Insulin makers accused of price-fixing scheme
$180,000 price tag for Miami Twp. boy’s prescription
Million-dollar drug keeps local woman alive
How do prescription drug prices get set?
Do you have a tip or story about prescription drug prices?
Contact Katie Wedell at kwedell@coxohio.com, (937) 328-0353, @KatieWedell.
You can also leave anonymous tips for the I-Team by calling (937) 225-2251.
About the Author