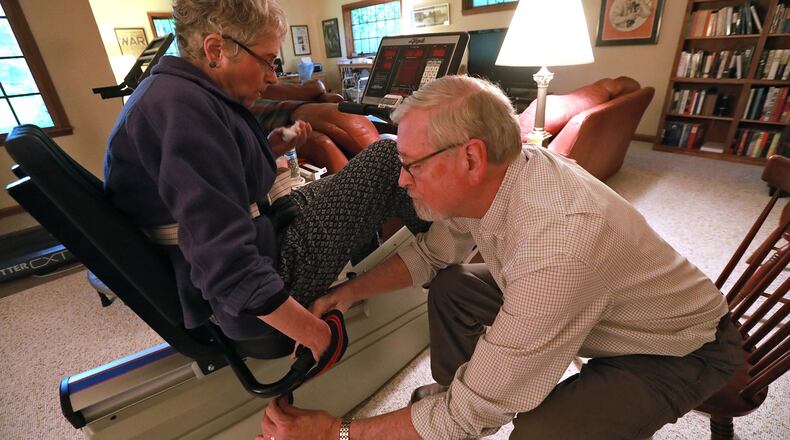
Acker quit her job roughly six years ago because juggling the care of her 93-year-old mother and her own health care became too much to handle.
“We hear this crisis about health care. The crisis that’s out there that nobody really wants to talk about is what are we going to do to continue to support this increasing population who has lost their abilities to do these everyday tasks?” said Doug McGarry, executive director of the Area Agency on Aging for west central Ohio.
Ohio has roughly 1.5 million family caregivers like Acker who provide nearly 1.4 billion hours of unpaid care a year, according to AARP Ohio, and that number will likely grow as the state’s over-65 population increases.
MORE: How to volunteer as a nursing home resident advocate
As a former hospice social worker, Acker of Xenia said she knows how to navigate the different resources for aging and caregiving support, but the job of caring for a family member is a consuming job. Family caregivers just can’t do it all, Acker said.
“You have all of their worries and all of your own worries,” Acker said.
Financial challenges
Steve Sidlo, who has been a caregiver for his wife, Cynthia, since her stroke 12 years ago, said even with insurance, he has significant out-of-pocket medical expenses related to her care.
“Last year it was somewhere in the neighborhood of $50,000,” Sidlo said.
Sidlo, a former Dayton Daily News managing editor, said he has a long-term care insurance policy that he estimates has paid out $300,000 so far, but he still has other uncovered expenses, mostly for help from several home health workers, which charge about $22 an hour.
He said he is fortunate to be able to afford regular in-home help.
“If I didn’t, I don’t know what the heck I do. … You’re doing every single thing. And and after a while you just you can’t keep it up,” Sidlo said.
Caregiving is expensive and can mean home modifications, in-home help, therapy and other out-of-pocket medical costs. Because of the time commitment, a family member sometimes has to leave their job or scale back hours so they can help out.
MORE: Dayton Children's opening first inpatient mental health unit
“There’s often a depletion of savings or dipping into children’s education funds. So some sort of stipend for caregivers I think would be really useful,” said Emily Muttillo, applied research fellow at Center for Community Solutions, a Cleveland-based think tank focused on health and human services.
Medicaid, which covers low-income and some disabled Ohioans, can pay for needed long-term care, such as a nursing home or PASSPORT, which covers care in the home.
The local Area Agency on Aging can do a free in-home assessment and figure out what support programs a person needs and qualifies for. McGarry, with Area Agency on Aging, said people often become caregivers little by little, slowly taking on more tasks such as chores and transportation.
There are more options for making a caregiving plan when his agency works with someone early, but they often meet with someone for an assessment after a crisis happens that makes the caregiver realize how much they’ve taken on. For example, the caregiver might have their own health care crisis, and realize how many tasks they were performing that now need taken over.
“It starts out small, and gradually builds to the point where it totally consumes your life,” McGarry said.
The needs, eligibility and availability of services will be different for each family and different in each community.
With the help of the Area Agency on Aging, Acker’s daughter, who is also a nurse, is registered with Medicaid and gets paid for caregiving hours during the day.
There are some long-term care insurance options available, but many of the current available plans are far less generous than what was on the market a decade ago. Some of the insurance plans have ceased operations after paying out far more than anticipated.
AARP also has been championing bills pending before Congress that would provide a tax credit to defray some of the costs of caregiving.
Emotional challenges
Carolyn Bohler said when she was caring for her husband, John, who died July 2018 from Lewey Body disease, the emotional challenges were much more difficult to figure out than figuring out the money.
It was hard to ask for help and she said it meant a lot when friends saw help was needed and reached out.
It was also difficult when John needed more care than she could give, but he also did not want to move out of the home.
Bohler, a retired Methodist pastor and Dayton resident, said that after years of being his caregiver, it had gotten to be too much to manage even with the help of Comfort Keepers coming in the mornings several days a week. He was 6 feet 3 inches tall and she is 5 feet 3 inches tall, which made it too much physically for her to help him get dressed and showered.
When she and her daughter eventually sat down with John to lunch and Carolyn said she needed him to move to an assisted living facility, he said no.
“It was traumatizing for me, because I didn’t know what to do,” she said.
They ended up finding solution that lasted for a while when they started paying for Comfort Keepers to come in both the mornings and the evenings, and eventually he did agree to move to Sanctuary at Wilmington, where she said he received great care.
It’s common for caregivers to feel stressed, guilty, frustrated or depressed as they manage caring for a loved one.
MORE: New crisis care center called missing piece for addicts
There are support groups and other resources to help caregivers with their personal wellbeing. At a class called Powerful Tools for Caregivers, hosted at Kettering Health Network, peer instructors help family caregivers through a free six-week course.
The course helps caregivers take care of themselves, set goals, problem solve, make tough decisions and reduce guilt and stress. The course also helps caregivers learn how to communicate effectively with family, doctors and paid caregivers.
Kelli Davis, program coordinator with Kettering Health Network Community Outreach, said they started the program in 2016 as a pilot with a grant through Area Agency on Aging.
The class helps caregivers build confidence, deal with stress, communicate with paid caregivers, make tough decisions, and learn what kind of resources are available. When the class starts, attendees are often a little anxious about the class, but as the weeks progress, they start to share how they are feeling as caregivers.
“Maybe for the first time they share how exhausting it is,” Davis said.
She said by week three the class starts to feel like a support group and participants start to identify outlets to take care of themselves, like by setting up a lunch date or starting to work out. After the class, members are encouraged to exchange information and stay in touch.
The class is designed for caregivers of someone with chronic illness and it has broadened over time to include a series for caregivers of children with special needs or behavioral needs and in the fall they will start a class for military caregivers. Davis said they are also starting a class where participants can join from at home over their computer.
Muttillo said family caregivers could use more access to emotional support services, particularly when they first become a caregiver.
“A family caregiver is often unprepared for the enormity of the task. They experience a loss of freedom and a loss of self because all of their energy is now used to take care of another person,” she said. “They need to be able to talk those things through with someone who is not going to judge them.”
Family caregiving also sometimes brings out family rifts and means difficult conversations.
An adult child caregiver for her mother might say she’s stretched thin and its time to move to an assisted living center, but her mother might not want to leave the home. A wife might insist to her husband that paid help is needed but her husband might not want a stranger in the home.
Heston said good communication is important at these times, though some of these conversations are going to be hard no matter what.
“I haven’t come up with an easy solution to that,” she said.
Sidlo had to learn a new reality where his wife — longtime word lover and librarian — had trouble with saying more than a couple words and couldn’t be home alone. Sidlo said he has a good support system and in recent years he also started seeing a counselor, which has been helpful.
“It’s really helpful to be able to talk your way through some of the things you end up dealing with … feelings of anger or frustration. So I know that’s really helped me to just cope with all this over the years,” he said.
Even when there’s frustration with the situation, there’s still love. Just a different way to express it and spend time together.
Sidlo pointed to jars of a specialty skin care line, Murad, and the jars found around their Springfield home. The product is almost more of a hobby for Cynthia than a product.
“She’s 72 years old and she really looks beautiful. She tells me to order these things on Amazon. It’s like $68 and you get like an ounce, but that’s her thing and I say yes ma’am,” Sidlo said.
What’s not here
Jennifer Heston, with Scripps School of Gerontology at Miami University, who has researched family caregiving, said when policy makers and agencies create programs, they often create programs shaped around the person needing care. But these programs should also take into account the needs of the caregiver and look at caregiver’s incomes and abilities as well when considering eligibility, she said.
That’s because programs like meals-on-wheels or vouchers for home health aides don’t just help older adults they are serving, but they also relieve the family caregivers who otherwise would need to meet those needs.
“For our state programs, we don’t always have a conversation that includes the caregiver as well to find out what it is that they really need,” Heston said.
Some experts also said there should be more supports for caregivers so they know learn the medical skills they need to have to help a family member, which can range from medication administration, to lifts and transfers, to wound care.
Family members do receive training during discharge from a hospital, as required by a 2017 Ohio law. Muttillo said this requirement was important but family members could still use in-home training on how to perform these tasks.
“To go to a class and learn it or to learn it during discharge is not the same as someone was in the home walking somebody through how,” Muttillo said.
Sidlo said he and the couple’s friend read up on the many medications Cynthia takes and he’s read all kinds of books on strokes. He now has a broad medical vocabulary and carefully reads through the never ending bills to make sure he doesn’t pay for anything twice.
“A lot of this stuff is so complicated, if you’re old and frail and especially if you have some dementia and you’re doing this yourself, you’re doomed. It’s really hard to keep up,” Sidlo said.
Muttillo said family caregivers would also benefit if there was better information to help them review whether a home health or personal care agency provides a good service or has had some violations. For now, its hard for consumers to find good quality measures.
High turnover in the industry also creates challenges because that can mean having to go through this trust building process over and over again.
“Until you are in that situation, you don’t understand what that really means. You are enabling someone to have their hands on your loved one and to provide the most intimate of care and that person starts out as a stranger,” Muttillo said. “To build up that level of trust takes time and there’s often high turnover in these positions.”
Where to get help
Area Agency on Aging
Request a free in-home assessment by the Area Agency on Aging to determine eligibility for programs and other community resources. Residents of Clark, Greene and Montgomery counties can call 223-HELP or 800-258-7277, or email aaa@info4seniors.org. Residents of Champaign, Darke, Logan, Miami, Preble and Shelby counties can contact Catholic Social Services of the Miami Valley at 800-521-6419 or email referrals@cssmv-sidney.org.
Powerful Tools for Caregivers
Powerful Tools for Caregivers is an educational workshop for people who are taking care of a family member or friend. It uses evidence-based curriculum designed specifically to support the family caregiver and improve his or her well-being. Call (937) 558-3988 to learn about dates and locations and to register for one of the classes at Kettering Health Network.
There are also volunteer opportunities to help with the program. Call (937) 558-3988 to learn more.
Caregiver Assistance Network support groups
• St. Susanna, 616 Reading Road, Mason. Meet in the church undercroft on the fourth Wednesday 7 to 8:30 p.m.
• Doverwood Village, 4195 Hamilton-Mason Road, Fairfield Twp. Meet in the chapel room on the second Friday 10 to 11:30 a.m.
Register before attending your first resource meeting by calling the Catholic Charities of Southwest Ohio CAREline at (513) 869-4483. For more information, go to ccswoh.org/caregivers. The resource groups help caregivers learn to care for themselves and access resource information, express their feelings in a non-threatening, and non-judgmental atmosphere and learn that they are not alone and to share techniques for handling the “nitty-gritty” of daily care.
Alzheimer’s Association supports
Alzheimer's Association has a 24/7 Helpline is at 1-800-272-3900, where professionals provide free support and caregivers can learn more about local programs and services as well as get information about legal, financial and care decisions. The helpline is for people living with Alzheimer's or other dementia, caregivers, families and the public.
The local chapter hosts free support groups for caregivers of those with Alzheimer’s and other forms of dementia. For more information or question about support groups, including early stage groups, call 1-800-272-3900. There are groups in Champaign, Clark, Darke, Greene, Miami, Montgomery and Shelby counties.
A telephone caregiver support group meets 7 p.m. on the first Monday of the month. Call Dawn Boroff at 937-610-7016 to register.
About the Author